Education,Macular Degeneration
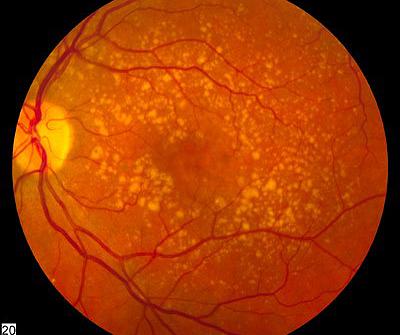
What is Age-Related Macular Degeneration (AMD)?
Age-related Macular Degeneration (or AMD) is a devastating eye disease. It is the leading cause of blindness in people 55 years and older in America.1 It causes blindness in about 1 million Americans, and with the aging of our country’s population, that number will only increase. We worry about our loved ones with the disease and about how we can best support them. What can I do to help my loved ones living with the disease? And what can I do to decrease the risk of having vision loss from AMD myself? This blog post will try to clarify and demystify the disease.
There are two forms of AMD: dry and wet. An analogy to understand these two forms is to think of your retina like a garden.
- Dry AMD is when there is a patch of dry soil where the plants (representing your eyes’ photoreceptors) have trouble growing. The plot there is thin and slowly over time, fewer and fewer plants grow.
- Wet AMD is the sudden eruption of a geyser through the soil, soaking the garden in a water and turning it into a swamp. As opposed to the dry form, now the plants cannot grow because they are submerged in water, so to speak. Vision also becomes blurry, as though looking through water.
There are ways of understanding if you are at risk for developing AMD. Many of these risk factors and associations are things that you cannot change. These include being Caucasian/white, female, and having a light-colored iris. Perhaps obvious, the disease also increases in prevalence with age, where the prevalence rises from about 1-2% at 60-69 years old to 7-12% from age 80 and over.2 There is also a strong contribution from genetics and family history, where studies have shown an increased odds of 4 to 6 times higher with a known family member.
Prevention of AMD
Prevention of AMD is primarily centered around reducing oxidative stress to the retina.
One of the primary causative links to AMD is smoking. We know that smoking is directly responsible for a whole body increase in oxidative stress, so not just to the lungs, but also the eyes and the retina. For those with at least a 10 pack-year history (which translates to smoking 1 pack a day for 10 years), the odds were 1.55 to 3.58 times higher of having AMD, depending on the study.2 Although difficult, quitting smoking can be one of the most important means of preventing AMD.
A second source of oxidative stress to the retina is ultraviolet (UV) light exposure. Studies suggest that wearing sunglasses can reduce the development of AMD. The data to support this claim is not supported as strongly as for smoking. Furthermore, although cataracts prevent clear vision, they partially block UV light from reaching the retina, so it is even more important for those after cataract surgery to wear sunglasses.
A third source of oxidative and inflammatory stress to the body is obesity. Studies have shown that those with a higher body mass index (BMI) above 30 kg/m have an increased risk of developing AMD than those with a normal body mass index. Those with a higher body mass index may also have other cardiovascular risk factors, like increased cholesterol or high blood pressure, and some studies have found correlations to AMD with these diseases as well.
A studied and proven method of delaying the progression of AMD is taking AREDS vitamins. Clinical trials showed that taking these vitamins daily can slow the progression of AMD for those with intermediate or late stages of the disease by about 27% over 5 years.3 It did not show any benefit for those without AMD or those with early AMD. It is important to check with your eye doctor about the stage of the AMD to determine if AREDS vitamins would be helpful. Daily multivitamins and a normal diet are not sufficient for the same effect that AREDS vitamins provide. For example, you would have to eat 7 to 8 oranges per day to get as much vitamin C as there is in a daily dose of the AREDS or AREDS2 formulation. There are also two formulations of AREDS vitamins: AREDS and AREDS2. Both formulations have vitamin C, vitamin E, and zinc, but the difference is that AREDS contains beta carotene, and AREDS2 contains lutein and zeaxanthin. For most, AREDS2 is a better formulation, both because it is better at reducing progression of AMD, and because people who smoke or used to smoke who took the original AREDS formula had increased risk of lung cancer.
Treatments for Wet AMD
Treatment to improve vision for AMD is currently only available for the wet form. These treatments come in the form of injections into the eye of a medication containing a substance that prevents the accumulation of fluid in the retina, called anti-vascular endothelial growth factor (anti-VEGF) agents. There have been many studies demonstrating their benefit, with many patients requiring multiple injections to adequately control their disease. As the focus of this article is prevention, I will not go more in depth at this time.
Research in Dry AMD Treatment
Given the burden of dry AMD, there are tremendous efforts in research to develop a therapy to reduce or prevent the disease. An area of the retina that “dries,” thins, and begins to lose function is called “geographic atrophy,” because in advanced forms it often looks like a state, country, or continent with distinct borders when viewed during an exam by your doctor. No treatment exists for reducing geographic atrophy.
One promising treatment that is currently in clinical trials is the drug pegcetacoplan. This drug plays a role in body’s immune system, specifically in what’s called the body’s “complement” system. The body normally uses the complement system to help it to label pathogens for destruction. Normally, this process is tightly regulated, but there appears to be a dysregulation of this process that is involved in AMD, where the complement system is targeting retinal tissue. The process is complex, and its role in development of AMD is incomplete and not entirely understood. However, the drug pegcetacoplan targets a molecule in the complement system (called C3) which can result in a slowing of development of geographic atrophy. A phase 2 clinical trial showed a 29% reduction in growth of geographic atrophy over 1 year.4 Given the devastating affect of geographic atrophy with no current treatment, this is exciting news, and we await future clinical trials of this drug and others as potential treatments.
What we offer at EANW for AMD
We are well-equipped at Eye Associates Northwest to care for patients with and at risk for AMD.
For those at risk of AMD, we offer full exams to track for the development of the disease, including dilated exams and optical coherence tomography (OCT) imaging. We are prepared to discuss the risk factors above with you to determine how you can best reduce your chances of developing AMD in your lifetime, especially if you have a family member who has the disease.
For those who have AMD, we have the means to follow your disease, discuss how to prevent its progression, and in cases of wet AMD, to treat it. AMD can be followed with various forms of retinal imaging at regularly scheduled visits made with your doctor. Furthermore, you can use an Amsler grid at home to learn look for subtle changes that could suggest that your AMD is changing, or converting from the dry to the wet form. Finally, we offer anti-VEGF injections for patients with wet AMD to help resolve or minimize fluid, which can help improve your vision.
Finally, there are many low vision devices that patients can use to improve their vision, even if it has been reduced by AMD. AMD primarily impacts central vision, decreasing both acuity of vision and contrast sensitivity. Low vision devices include magnifiers (both stand-alone lenses, and electronic devices), various hues of sunglasses that help to improve contrast sensitivity, and different types of lamp lights to improve vision around the house. There is not a one size fits all regimen that works for every patient.
Conclusion
AMD is a devastating disease. Some things that you can do to prevent development of AMD are: quit smoking, wear sunglasses, and maintain a healthy body weight. If you have signs of intermediate or advanced AMD, AREDS2 vitamins are beneficial. Taking these preventive steps are especially helpful in patients who have a positive family history, where the lifetime risk of the disease is higher.
– Ryan P. Lange, MD
Citations
1. Chakravarthy, U., Wong, T.Y., Fletcher, A. et al. Clinical risk factors for age-related macular degeneration: a systematic review and meta-analysis. BMC Ophthalmol 10, 31 (2010). https://doi.org/10.1186/1471-2…
2. Wong, I.Y.H., Koo, S.C.Y. & Chan, C.W.N. Prevention of age-related macular degeneration. Int Ophthalmol 31, 73–82 (2011). https://doi.org/10.1007/s10792…
3. The Age-Related Eye Disease Study Research Group (2001) A randomized, placebo-controlled, clinical trial of high-dose supplementation with vitamins C and E, beta carotene, and zinc for age-related macular degeneration and vision loss. AREDS Report No. 8. Arch Ophthalmol 119:1417–1436
4. Liao DS, Grossi FV, El Mehdi D, Gerber MR, Brown DM, Heier JS, Wykoff CC, Singerman LJ, Abraham P, Grassmann F, Nuernberg P, Weber BHF, Deschatelets P, Kim RY, Chung CY, Ribeiro RM, Hamdani M, Rosenfeld PJ, Boyer DS, Slakter JS, Francois CG. Complement C3 Inhibitor Pegcetacoplan for Geographic Atrophy Secondary to Age-Related Macular Degeneration: A Randomized Phase 2 Trial. Ophthalmology. 2020 Feb;127(2):186-195. doi: 10.1016/j.ophtha.2019.07.011. Epub 2019 Jul 16. PMID: 31474439.
